Diabetes poses a significant threat to public health in China. Type 1 diabetes, which typically affects children and adolescents, presents unique challenges. Traditional islet transplants are effective but limited by a severe shortage of donors. Consequently, achieving large-scale islet regeneration has become an urgent global challenge. Now, a breakthrough in stem cell therapy for Type 1 Diabetes offers a promising solution.
A Breakthrough in Stem Cell Therapy for Type 1 Diabetes
The Chinese Academy of Sciences recently announced a major achievement. The Center for Excellence in Molecular Cell Science, in collaboration with Shanghai Changzheng Hospital, successfully performed minimally invasive transplants using regenerated islets. Specifically, they utilized both autologous and allogeneic stem cells. This achievement successfully restored islet function and autonomous blood sugar regulation in patients. The related findings were published in the prestigious journal *The Lancet Diabetes & Endocrinology*.
Clinical Results and Implications
This exploratory study involved three patients with Type 1 diabetes. It achieved positive outcomes, including islet function reconstruction and the ability to discontinue exogenous insulin. However, the study also indicated a need for long-term immunosuppressive therapy. This is necessary to overcome the recurrence of autoimmune issues associated with Type 1 diabetes.
According to Cheng Xin, the lead researcher, in vitro islet regeneration is akin to “replacing parts” for the human body. The team established a new technical system based on endoderm stem cells. Furthermore, this new approach simplifies the differentiation steps and shortens the production cycle to just two weeks. Importantly, these endoderm stem cells do not proliferate in the body, significantly reducing the risk of tumor formation. For more scientific details, refer to the official publication in The Lancet .
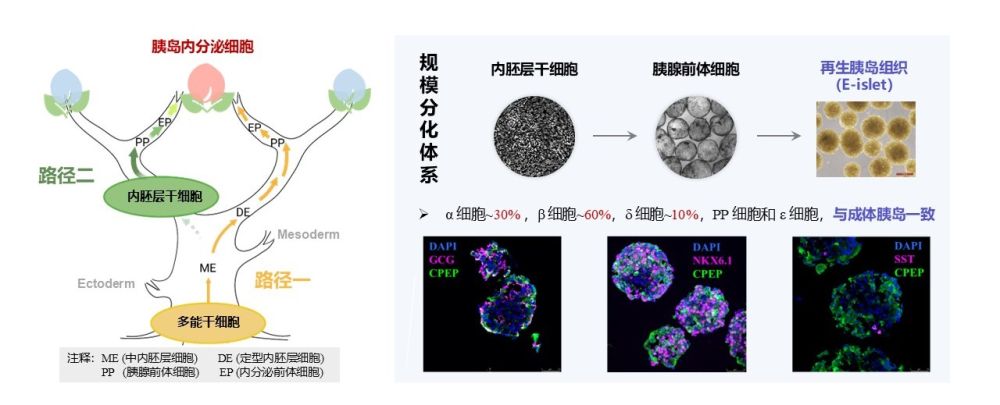
How the Regenerated Islets Work
Using in vitro directional differentiation technology, the team constructed “regenerated islets.” These are designed to treat severe islet dysfunction or failure. Doctors transplant these regenerated islets via hepatic portal vein infusion. Once transplanted, they function like normal islet tissue to regulate blood sugar.
Future Applications
Based on independent intellectual property rights, the team developed “Allogeneic Human Regenerated Islet Injection (E-islet01).” This innovation received Investigational New Drug (IND) approvals from both Chinese and US regulatory authorities. Therefore, this breakthrough marks a significant step forward in stem cell therapy for Type 1 Diabetes. Relevant clinical trials are now proceeding in an orderly manner.
Executive Editor Wang Xue